At its core, trauma-informed care training is about a fundamental shift in perspective. It's a learning process that teaches professionals and organizations to move away from asking, "What's wrong with you?" and instead, to gently and curiously ask, "What happened to you?"
This training gives people the knowledge and practical tools to recognize just how widespread trauma's impact is. With that understanding, they can start building environments that actively support healing and, just as importantly, avoid causing further harm.
What Is Trauma-Informed Care and Why Does It Matter?
Let's be clear: trauma-informed care isn't a specific type of therapy or a clinical checklist. Think of it more as an operating system—a complete change in how we approach our work and interact with others. It's like swapping an old, inaccurate map that often leads to dead ends for a modern GPS that understands the terrain. The old map might have led us to blame people for their behaviors, but the new, trauma-informed map helps us see the life experiences that shaped those responses in the first place.
This approach starts with the recognition that trauma is far more prevalent than most of us realize. The ripple effects show up everywhere—in doctors' offices, classrooms, libraries, and workplaces—often in ways that are easily misinterpreted. A patient who repeatedly misses appointments isn't necessarily being "non-compliant"; they might be wrestling with anxiety triggered by medical settings. A student who acts out in class isn't just "defiant"; their behavior could be a direct reaction to a chaotic and unsafe home life.
The Universal Design Analogy
A great way to understand the power of this approach is to think about universal design in architecture. Ramps and automatic doors were originally created for people using wheelchairs. But who else benefits? Parents pushing strollers, delivery people with heavy carts, and travelers dragging luggage. Everyone's experience is made easier.
Trauma-informed care works the same way. It creates emotionally and physically safe environments that are better for everyone. When an organization fully embraces this framework, the positive changes ripple out to benefit all clients, customers, and staff, not just those with known trauma histories.
A trauma-informed environment fosters a sense of physical and psychological safety for everyone. It acknowledges that people's life experiences shape how they engage with services and that creating a supportive space is a universal need, not a specialized accommodation.
A Foundational Shift for Every Profession
Adopting this perspective is critical because the effects of unresolved trauma can cast a long shadow over a person's health, behavior, and overall well-being. Recognizing this link is changing how we think about everything from healthcare to education.
In fact, extensive research shows that workforce development through trauma-informed care training is one of the most effective ways to improve professional competency. This is an urgent need, especially when you consider a massive World Health Organization study across 24 countries, which found a staggering 70.4% lifetime trauma prevalence. You can dig deeper into the research on clinician training and global trauma prevalence to see the full scope of the issue.
These numbers make it clear that this isn't just for therapists anymore. It's an essential framework for anyone in a people-facing role—doctors, teachers, HR managers, librarians, and community leaders. It provides the skills to build trust, empower individuals, and create the conditions for genuine healing and growth.
Before we go deeper, it's helpful to see a direct comparison of these two approaches. The table below highlights the key differences in mindset and action between a traditional model and a trauma-informed one.
Shifting Perspectives From Traditional Care to Trauma-Informed Care
| Aspect | Traditional Approach (Asks 'What's wrong with you?') | Trauma-Informed Approach (Asks 'What happened to you?') |
|---|---|---|
| Focus | Diagnosing symptoms and deficits. | Understanding the whole person and their experiences. |
| Behavior | Viewed as intentional, manipulative, or pathological. | Seen as an adaptive coping mechanism for survival. |
| Power Dynamic | Hierarchical; the provider is the expert. | Collaborative; power is shared to foster agency. |
| Goal | Compliance and symptom reduction. | Healing, empowerment, and building resilience. |
| Safety | Assumes physical safety is sufficient. | Prioritizes physical, psychological, and emotional safety. |
| Key Question | "What's wrong with you?" | "What happened to you, and what do you need to feel safe?" |
As you can see, the shift is profound. It moves from a model that can feel judgmental and pathologizing to one rooted in compassion, understanding, and collaboration. This change is at the very heart of creating services that truly serve people.
The Six Core Principles of a Trauma-Informed Approach
To truly bring a trauma-informed model to life, an organization needs to be built on a solid foundation. That foundation rests on six core principles, championed by leading health organizations like the Substance Abuse and Mental Health Services Administration (SAMHSA) and the CDC. These aren't just buzzwords on a poster; they are the active ingredients that create an environment where everyone—staff and clients alike—can feel secure and begin to heal.
Think of these principles as the essential pillars holding up a bridge. If even one is weak or missing, the whole structure becomes unstable. Good trauma-informed care training is all about teaching people how to build and reinforce these pillars in every single interaction, creating a safe passage for those they serve.
This shift in perspective is about moving from a system that can accidentally re-traumatize people to one that actively promotes healing and safety.
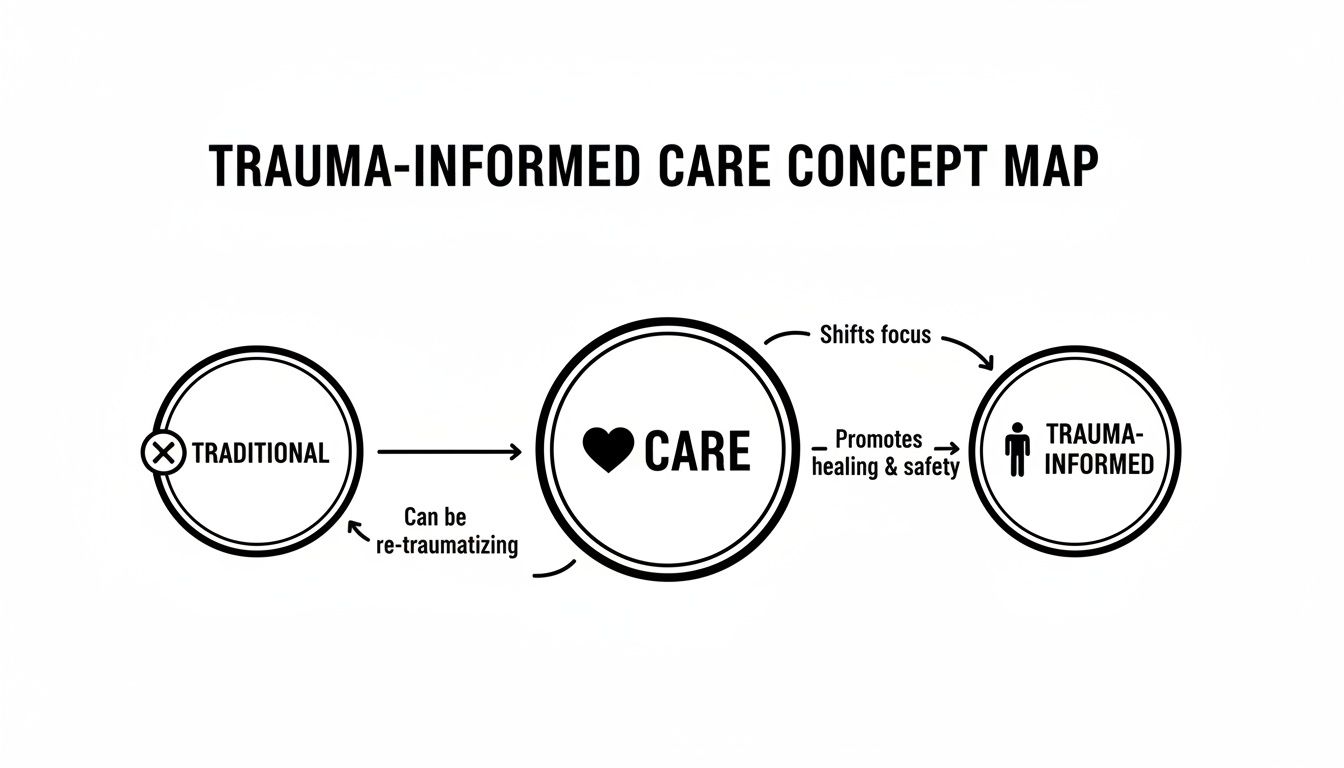
As the map shows, the focus moves away from just managing symptoms and toward understanding the whole person, which ultimately leads to a more supportive and effective way of providing care.
1. Safety
The first and most fundamental principle is Safety. This is about so much more than just well-lit parking lots. It's about creating an atmosphere of psychological and emotional safety where people can let their guard down, knowing they won’t be met with judgment or threats.
For someone who has experienced trauma, the world often feels like a dangerous and unpredictable place. A calm, welcoming environment—think softer lighting, comfortable chairs, and clear, friendly signage—can make a world of difference. It’s all about intentionally designing spaces and interactions that lower a person’s stress response instead of raising it.
2. Trustworthiness and Transparency
Once safety is established, the next step is building trust. This principle is all about operating with complete transparency. For many trauma survivors, trust was shattered by the very people or systems that were supposed to protect them.
Rebuilding it means being upfront and clear in every interaction. A doctor might walk a patient through every step of an exam before they begin. A manager might clearly lay out roles and expectations before a new project starts. When you demystify the process and make interactions predictable, you create reliability. That's how trust begins to grow again.
3. Peer Support
This principle recognizes the incredible power of shared experience. Peer support brings people with lived experience of trauma into the fold as mentors, advocates, and beacons of hope. They offer a level of empathy and genuine understanding that is difficult for others to replicate.
Peer support is a game-changer because it proves that recovery is real. It shifts the conversation from "What's wrong with you?" to "I've been where you are, and I know you can get through this."
Seeing someone who has navigated a similar journey can instantly dissolve feelings of isolation and inspire a belief in what's possible. It’s a powerful reminder that connection is a key part of healing.
4. Collaboration and Mutuality
Here, we level the playing field. The old, top-down model where an "expert" tells a client what to do just doesn't work in a trauma-informed world. Instead, this principle emphasizes partnership and shared decision-making. It operates from the belief that every person is the true expert on their own life.
In practice, this looks like a case manager co-creating a support plan with a client, not for them. It’s about ensuring power is shared and respected, valuing every person's insight, and working together toward a common goal.
5. Empowerment, Voice, and Choice
Hand-in-hand with collaboration, this principle is about recognizing and amplifying an individual's strengths. It’s about creating real opportunities for people to have a say in their care and to make choices that feel right for them.
Trauma often robs people of their sense of control. The simple act of providing choices helps restore that agency. It can be as small as asking, "Would you prefer this chair or the one by the window?" or as profound as letting a client define their own goals in a treatment program.
6. Cultural, Historical, and Gender Issues
Finally, a trauma-informed approach demands that we move beyond stereotypes and biases. It requires us to understand and address the deep-seated historical and generational trauma that impacts entire communities. It also means recognizing the unique ways gender can influence a person’s experience of trauma.
This principle challenges organizations to become truly responsive to the racial, ethnic, and cultural needs of the people they serve. It’s about offering services that are not just available, but are delivered with cultural humility—acknowledging the systemic forces that can create and sustain trauma in the first place.
What You'll Learn in a Trauma-Informed Care Training Program
Stepping into a trauma-informed care training program is a bit like learning a new language. You aren’t just handed a list of vocabulary words—the theories and concepts. You learn the grammar, the cultural context, and the etiquette—the practical skills—that allow you to connect with people with genuine understanding and compassion.
A truly great curriculum gets you out of your chair and into experiential learning that builds real confidence. It pulls back the curtain on the science of trauma and hands you a clear roadmap for putting the principles into practice. The goal isn't just to know about trauma-informed care; it's to know how to be trauma-informed in your everyday work.

Core Curriculum Components
While every program has its own unique flavor, any comprehensive trauma-informed care training will be built on a few essential pillars. Think of them as building blocks that work together to create a deep, functional understanding of how to make this approach a reality.
You can expect to dive into key learning areas like these:
- The Neurobiology of Trauma: This is where you get a look "under the hood" at how traumatic experiences physically change the brain. You’ll see how the body's stress response system can get stuck in high gear, leading to behaviors that are too often mistaken for defiance or apathy.
- Recognizing the Signs of Trauma: Participants learn to see the sometimes subtle, sometimes obvious signs that someone is carrying the weight of trauma. It's about understanding how these signs can show up differently across ages, cultures, and life experiences.
- Applying the Six Principles in Real Life: This is where the rubber meets the road. The training will focus on how to actively use the core principles—Safety, Trustworthiness, Peer Support, Collaboration, Empowerment, and Cultural Humility—in everyday interactions.
- Preventing Re-traumatization: You’ll learn to spot common triggers and unintentional actions that can re-injure someone. This could be something as seemingly small as an abrupt change in schedule, the tone of your voice, or even the layout of a room.
- Communication and De-escalation Skills: This part of the training gives you specific techniques for communicating in a way that builds trust and helps calm tense situations, keeping everyone—staff and clients alike—safe.
A core tenet of effective training is the shift from a problem-focused mindset to a strengths-based one. It teaches you to see an individual's resilience and coping mechanisms, not just their symptoms or challenges. This simple change fundamentally alters the dynamic of care.
Experiential Learning and Skill Building
The most powerful training experiences happen far away from a PowerPoint presentation. They rely on interactive methods that help you internalize the concepts and build muscle memory for new ways of responding. It's the difference between reading a cookbook and actually making the meal. One gives you knowledge; the other builds a skill.
These hands-on learning methods are what build real-world confidence:
- Role-Playing Scenarios: You'll act out challenging but realistic situations, like responding to a client's sudden distress or navigating a difficult team conversation. This gives you a safe space to practice empathy and de-escalation without real-world consequences.
- Case Study Analysis: Working in groups, you'll dissect detailed case studies to spot trauma responses, brainstorm trauma-informed interventions, and debate the best course of action. It's a fantastic way to develop critical thinking and problem-solving skills.
- Reflective Practice: Good training carves out dedicated time for self-reflection. This helps you look at your own biases, assumptions, and emotional reactions, which is a critical step in preventing burnout and providing better care.
Understanding Vicarious Trauma and Self-Care
Finally, no trauma-informed care training is complete without a serious focus on the well-being of the provider. Hearing difficult stories and witnessing suffering day after day takes an emotional toll. There's a name for it: vicarious trauma, or secondary traumatic stress.
A high-quality program will teach you to recognize the signs of vicarious trauma and burnout in yourself and your colleagues. More importantly, it will give you concrete, practical strategies for building personal resilience and practicing sustainable self-care. This ensures that the people doing this vital work can keep doing it effectively and compassionately, without sacrificing their own health in the process.
How Trauma-Informed Practices Look in the Real World
It's one thing to talk about theory, but what does this training actually look like from day to day? The real power of a trauma-informed approach isn't found in a textbook; it’s in the small, intentional shifts people make in how they interact with others. These aren't complicated or expensive changes. They are fundamentally human adjustments that build trust, prevent re-traumatization, and can dramatically improve outcomes for everyone involved.
Whether you're in a doctor's office or a corporate boardroom, the applications are universal. The core ideas of safety, trust, and empowerment become real actions that help people feel seen, heard, and respected. Let's look at some concrete examples of how this works across different fields.

Application in Healthcare and Dental Settings
For a lot of people, medical and dental settings are inherently stressful. The unfamiliar sounds, the physical vulnerability, and the fear of bad news can easily trigger a trauma response. A professional trained in this approach understands this and adjusts how they work.
Imagine a doctor who needs to perform a procedure. Instead of just starting, they pause to explain every single step, describe what the patient will feel, and then say, "You are in control here. If you need me to stop at any time, just raise your hand." That simple statement gives the patient a sense of agency—something trauma so often strips away.
In a dental office, a hygienist might notice a patient’s shoulders tense up as the chair leans back. Rather than pushing through, they might say, "I'm going to recline the chair now. Please let me know if this angle is uncomfortable for you." They eliminate surprises and create a predictable, safe experience. These small gestures can mean the difference between a patient who gets the care they need and one who avoids the dentist for years out of anxiety. With research showing that as many as 70% of adults in the U.S. have experienced at least one traumatic event, these practices are absolutely essential.
Transforming Education and Classrooms
Schools are another critical environment for a trauma-informed lens. A child dealing with chaos at home might struggle to focus in class. A traditional mindset might label that child "disruptive," but a trauma-informed teacher sees a child stuck in survival mode.
Here’s what that looks like in practice:
- Predictable Routines: The teacher creates a consistent daily schedule and posts it where everyone can see it. For a child whose home life feels out of control, this predictability creates a profound sense of safety.
- Calm-Down Corners: Instead of punitive timeouts, the classroom has a "calm-down corner" with soft pillows or quiet activities. This teaches a child how to self-regulate, rather than just punishing them for a stress response.
- Offering Choices: Throughout the day, the teacher offers simple choices: "Would you like to work at your desk or on the floor with a clipboard?" This helps restore a feeling of control.
These strategies don't just help one child; they make the entire classroom a more stable and supportive place for everyone to learn.
The essence of trauma-informed care is recognizing that behavior is communication. When we get curious about what that behavior is trying to say—often a need for safety, connection, or control—we can respond with compassion instead of judgment.
Enhancing Social Services and Community Support
Social service agencies are on the front lines, often working with people at their most vulnerable. Applying trauma-informed principles here is non-negotiable if you want to build the trust needed to actually help.
Think about a case manager working with someone experiencing homelessness. Instead of handing them a rigid, one-size-fits-all plan, they start a conversation.
They might ask, "What do you feel is the most important thing for us to tackle first?" or "What do you need from me to feel safe and respected when we meet?" This approach honors the principle of Collaboration and Mutuality, treating the client as the expert in their own life. It completely changes the power dynamic from a top-down hierarchy to a true partnership, fostering dignity and motivating people to engage. This shift is at the heart of so many inspirational stories of the human spirit, where simply feeling heard becomes the catalyst for life-altering change.
Fostering Psychological Safety in the Workplace
The principles of trauma-informed care training aren't just for "helping" professions anymore. They're quickly becoming a cornerstone of what makes a healthy and productive workplace culture. A trauma-informed manager gets that employees bring their whole selves—including their personal histories and stressors—to work.
This might look like:
- Clear and Transparent Communication: Making sure that changes in roles or company direction are communicated with empathy, avoiding surprises that can trigger anxiety.
- Psychologically Safe Check-ins: Turning one-on-one meetings into genuine dialogues that start with questions like, "How is your workload feeling this week?" instead of just rattling off a to-do list.
- Flexible Policies: Recognizing that employees have full lives outside of the office and offering flexibility when possible to support their well-being.
When leaders prioritize psychological safety, they create an environment where team members feel secure enough to innovate, admit mistakes, and ultimately do their best work.
How Do You Measure the Real Impact of Trauma-Informed Training?
It’s one thing to complete a training course, but it’s another thing entirely to see it change how an organization actually works. The true value of becoming trauma-informed isn't just a feel-good moment in a workshop; it’s about the lasting, positive shifts that ripple through your entire team and the people you serve. While personal stories of change are incredibly powerful, the data backs them up, showing this is a sustainable strategy, not just a one-off event.
When your staff starts to see their work through a trauma-informed lens, their actions begin to subtly reshape the system itself. This isn't just theory. It leads to real, tangible changes—like rewriting policies to put psychological safety first, getting smarter about how resources are used, and building a workforce that feels more connected and resilient.
From a One-Day Workshop to an Everyday Practice
The goal of any good training is for the lessons to stick long after the slideshow is over. The evidence shows that a trauma-informed approach does exactly that. It doesn't just sit in a binder on a shelf; it gets woven into the fabric of a professional's daily practice. That’s where the magic really happens.
One landmark study brought this to life with some pretty staggering long-term results. Six months after the training, 96% of participants said they were still actively applying a trauma-informed lens to their work. Think about that for a second. Almost everyone. And 92% were using what they learned to concretely improve how they served their clients.
Even more telling, 64.2% reported that their organizations had started to overhaul resources and roll out new trauma-informed practices. It’s clear proof that individual learning sparks real, systemic change. If you're curious, you can dig into the full study on lasting trauma-informed change to see the data for yourself.
This shows that the principles don't just fade away. They become embedded in thousands of tiny, everyday interactions that, all together, create a fundamentally safer and more effective environment.
More Than Just Good Practice—It's a Smart Investment
Investing in your people with this kind of training pays dividends that go way beyond better client outcomes. One of the biggest payoffs is the direct impact it has on your workforce, especially in high-stress fields where burnout and turnover are constant, costly battles.
A trauma-informed workplace is simply a healthier workplace. When you build an environment on a foundation of respect, transparency, and psychological safety, you aren't just serving clients better—you're protecting your most valuable asset: your people.
When employees feel supported and have the right tools to manage the emotional weight of their jobs, the results speak for themselves.
- Less Staff Burnout: The training gives people practical tools to spot the signs of vicarious trauma and build sustainable self-care habits. This is a direct counterpunch to the emotional exhaustion that drives so many talented people out of their professions.
- Lower Employee Turnover: A psychologically safe workplace is a place people want to stay. When your team feels valued and understood, retention naturally goes up, saving you the immense cost and headache of constantly recruiting and training new staff.
- Higher Job Satisfaction and Morale: Feeling like you’re good at your job is a powerful morale booster. This training gives professionals the confidence to handle tough situations with skill, which leads directly to greater satisfaction and a more positive culture for everyone.
When you step back and look at the whole picture, the conclusion is clear. Trauma-informed care training isn't an expense; it's a strategic investment in building healthier, more compassionate, and more effective systems for every single person involved—from the clients walking through the door to the dedicated professionals who are there to help them. The benefits aren’t just immediate; they're foundational. They’re built to last.
How to Find and Choose the Right Training Program
Deciding to become trauma-informed is a huge step, and picking the right training program is your first big decision. The field is booming, which is great, but it also means you have to look past the slick marketing to find something that actually teaches you real skills, not just hands you a certificate.
Think of it this way: a good program should feel less like a lecture and more like a guided practice in building empathy and safety.
The sheer scale of this growth is a bit staggering. The global market for trauma-informed therapy services, which really fuels the demand for this kind of training, was valued at a massive $11.09 billion in 2025. It’s expected to hit $15 billion by 2033. You can dig into the numbers and see what this trend means for the therapy market. All this growth means more options for you, but it also puts the pressure on to choose wisely.
Key Questions to Ask Before Enrolling
To sort through all the options, you need a solid game plan. Treat this like a checklist to make sure your investment of time and money will pay off in a meaningful way. Before signing up for anything, get clear answers to these questions:
- Is the curriculum evidence-based? The training has to be built on a solid foundation of research, especially the neurobiology of trauma and the core principles laid out by respected organizations like SAMHSA.
- Does it include survivor perspectives? The most impactful training programs bring in the lived experiences of trauma survivors. This might be through peer support specialists or by making survivor stories central to the lessons, which keeps the content grounded and respectful.
- What kind of ongoing support is offered? A one-day workshop is just the start. Look for programs that provide follow-up coaching, peer consultation groups, or other resources. This helps you actually use what you've learned when you run into real-world challenges.
- Is the training interactive and skill-based? You can't learn this stuff by staring at a PowerPoint. The best training gets you involved with role-playing, case studies, and reflective exercises so you can practice new skills in a safe space.
Evaluating Training Providers
Once you've narrowed down your list, it's time to vet the providers themselves. A provider's background and philosophy are just as important as the syllabus. This is where you separate the true experts from those just jumping on a trend.
Look for facilitators who have deep, practical experience—not just teaching, but actually using trauma-informed principles in settings that match your own. Their ability to share real-world stories and troubleshoot tricky situations is worth its weight in gold.
The ultimate goal of any trauma-informed care training should be to build your capacity for compassionate curiosity. It equips you not with rigid scripts, but with a flexible, empathetic lens to better understand the people you serve.
Finally, see how much the program emphasizes self-care and preventing vicarious trauma. A responsible provider knows this work can take an emotional toll and will spend real time helping you build your own resilience. This focus on the well-being of the practitioner is a sure sign of a thoughtful, ethical program. If you're looking to build your own resilience, you might find some great resources in our collection of recommended nonfiction books for personal development.
Your Questions About Trauma-Informed Care Training, Answered
As you start to explore trauma-informed care, it’s completely normal for questions to pop up. This is a big shift in how we think about our work and interact with others, so getting into the practical details is key. Let’s walk through some of the most common questions I hear about this training.
How Long Does This Training Usually Take?
The honest answer? It varies—a lot. You’ll find everything from a quick 2-hour introductory webinar to an immersive multi-day workshop. Some certification programs can even span several months.
What's right for you really depends on what you're trying to achieve. A short overview might be perfect for raising general awareness across your entire organization. But for frontline staff who need to apply these principles every single day, a much deeper, skill-focused training is essential. The best models I've seen involve an initial training session followed by ongoing coaching to make sure the new practices actually become part of the culture.
Is This Training Only for Therapists?
Not at all. While the concept was born in the mental health world, we now understand its principles are vital for anyone in a people-facing role. The reality is that trauma's impact shows up everywhere.
That’s why this training is incredibly valuable for:
- Educators trying to create safe and stable classrooms where kids can actually learn.
- Healthcare professionals working to build trust with patients who may be anxious or scared.
- Human resources managers who want to foster a truly psychologically safe workplace.
- Librarians and community workers serving a public with incredibly diverse life experiences.
Simply put, if your work involves interacting with other human beings, this training is for you.
What Is the Difference Between This Approach and Trauma-Specific Treatment?
This is a really important distinction to grasp. I like to explain it with an analogy:
Trauma-informed care is like a universal precaution. It's the safe, supportive environment you create for everyone because you can’t know who has a history of trauma. Trauma-specific treatment, on the other hand, is the targeted medical intervention for someone with a known trauma-related diagnosis.
Training in trauma-informed care teaches you how to build that safe environment. It’s about adjusting your lens, your policies, and even your physical spaces to avoid re-traumatizing anyone. Trauma-specific treatments are clinical services—like EMDR or Trauma-Focused CBT—that are delivered by licensed therapists to help individuals process and heal from specific traumatic events. Both are critical, but they play very different roles.
How Can I Advocate for This in My Organization?
A great place to start is by tying the training directly to your organization’s mission. Frame it as a strategic investment that pays dividends, not just another line-item expense.
Bring data to the table. Show how a trauma-informed approach can reduce staff burnout, improve client satisfaction, and lead to better overall outcomes. You can share articles and case studies from similar organizations, or even suggest a small pilot program to demonstrate the impact firsthand. When people see the positive changes, it’s much easier to get their buy-in.
At Babette Wilson, we believe in the power of stories and resources that foster understanding and resilience. Explore insightful narratives and empowering guidance by visiting the Babette Wilson Author website.
Prepared with Outrank app


Pingback: hello world
Pingback: metoclopramide reglan
Pingback: finasteride topical
Pingback: diflucan for yeast
Pingback: prevacid 30 mg capsule
Pingback: misoprostol price for abortion
Pingback: cenforce 150 mg review
Pingback: xenical generic iskustva
Pingback: cenforce 100mg reddit
Pingback: semaglutida para que sirve precio similares
Pingback: fincar price
Pingback: bupropion dose sizes